Imagine you looked into the mirror and found your reflection staring back, not with just your eyes but also with acne prominently displayed on your face. It’s disheartening, isn’t it? In contrast, consider a picture-perfect portrait of clear skin. Love that mental image? What if we tell you that the elusive key to achieving this might be an unexpected hero – probiotics? Yes, the gut-health superheroes might be your ace against acne too!
But do probiotics really have what it takes to battle one of our most common skin foes? Or is this just another ‘scientifically-backed’ fad that promises much but delivers little? Dive in as we explore the latest research and unveil the compelling science behind why and how probiotics may potentially revolutionize how we combat acne.
Growing evidence suggests that probiotics can be an effective treatment for acne. Studies have shown that probiotics can improve gut health, reduce inflammation, and promote skin barrier repair, all of which may reduce acne symptoms. However, as with any treatment, results may vary depending on the individual and their circumstances. It is important to consult with a healthcare professional before starting any new supplement or treatment for acne.
Understanding Probiotics
When we hear “probiotics,” many think about yogurts and other fermented foods. However, probiotics are much more than just a trendy food item. Probiotics refer to the beneficial living bacteria that live in our gut and contribute to our well-being. They are crucial in maintaining good health by keeping harmful bacteria at bay and supporting proper digestion and nutrient absorption.
Probiotics are often described as the body’s friendly microbes. There are hundreds of different strains of probiotics, grouped under two primary categories: Lactobacillus and Bifidobacterium. Each strain uniquely contributes to the body, and scientists continue studying how they work.
An analogy that can help us understand this is when we compare gut bacteria to plants in the soil. When you want a plant to grow strong and healthy, you need nutrient-rich soil to promote its growth. Similarly, when your gut flora is balanced with beneficial bacteria like probiotics, it can help promote overall good health.
In addition to supporting digestive health, some research studies have shown that probiotics may be effective for preventing or treating a variety of conditions, including diarrhea caused by antibiotic use, irritable bowel syndrome (IBS), inflammatory bowel diseases (IBD) such as Crohn’s disease and ulcerative colitis, allergies, and even mental health issues.
However, not everyone agrees on the effectiveness of probiotics. Some experts argue that there isn’t enough evidence yet to support their use for some medical conditions like depression or autism spectrum disorder. This is why it’s important to consult with a healthcare professional before adding any type of supplement or dietary change.
Now that we understand probiotics let’s dive deeper into their role in the body.
- A 2018 review of studies published in the American Journal of Clinical Dermatology found that certain strains of probiotics can reduce skin inflammation, improve skin barrier function, and create a more balanced skin microflora which may contribute to reducing acne.
- According to data from the American Academy of Dermatology, acne is the most common skin condition in the United States, affecting up to 50 million people annually. Many of these individuals are now seeking alternative treatments such as probiotics.
- A double-blind study conducted by scientists at Seoul National University found that 54% of their subjects reported a significant reduction in their acne severity after taking Lactobacillus fermented kimchi and a low dose of Bifidobacterium breve for 12 weeks.
Probiotics are beneficial living bacteria in our gut that play a crucial role in maintaining good health by keeping harmful bacteria at bay and supporting proper digestion and nutrient absorption. They are often described as the body’s friendly microbes, with different strains like Lactobacillus and Bifidobacterium offering unique contributions to the body.
Additionally, probiotics may effectively prevent or treat conditions such as diarrhea caused by antibiotic use, irritable bowel syndrome (IBS), inflammatory bowel diseases (IBD) such as Crohn’s disease and ulcerative colitis, allergies, and mental health issues. However, it’s important to consult with a healthcare professional before adding any type of supplement or dietary change.
The Role of Probiotics in the Body
Our body is full of good and bad bacteria, which are essential to our health. When we have more good bacteria than harmful ones, our immune system strengthens and can fight infections and diseases better.
The primary role of probiotics in the body is to promote a healthy gut by keeping the bacterial balance in check. They do this by competing with harmful bacteria for space and nutrients in the gut. Doing so limits the growth of bad bacteria and promotes optimal digestion and nutrient absorption.
An analogy that can help visualize this is to imagine our gut as a garden bed. Just like a garden bed needs weeding to keep out unwanted weeds, it’s crucial to have enough “good” bacteria to ward off the bad ones. When you add “good” bacteria like probiotics to your gut, they act like a protective barrier keeping pathogens from growing out of control.
Recent studies have also suggested that maintaining a balanced microbiome (the collection of microorganisms that inhabit the body) benefits far beyond gut health. For example, gut-brain communication is gaining attention from researchers who find that probiotics may improve cognitive functions like memory and learning while reducing anxiety and depression symptoms.
However, some critics argue that many probiotic studies have been small or inconclusive. While these studies suggest positive correlations between probiotic use and many health conditions, further large-scale research studies are needed for full validation.
So what does this all mean for acne? Next, Let’s look at the scientific link between probiotics and acne.
The Scientific Link Between Probiotics and Acne
When it comes to understanding the scientific link between probiotics and acne, it is crucial first to grasp the concept of gut flora. The human digestive system is home to a vast ecosystem of bacteria, viruses, and fungi called gut flora. This internal environment is fundamental in maintaining many bodily functions, such as digestion, immunity, and metabolism. The balance of the gut microbiota is important for overall health and well-being. When this balance is disrupted, it can lead to various health issues, such as inflammatory skin conditions like acne.
Acne vulgaris is a chronic disease that affects millions worldwide, often resulting in skin eruptions like whiteheads, blackheads, pimples, blemishes, and cysts. Factors contributing to acne development include bacterial colonization, increased sebum production, hormonal imbalances, and abnormal keratinization of the sebaceous canals. Since intestinal microbiota plays a significant role in immune function, research has suggested that imbalance or dysbiosis in the gut microbial community could impact skin health.
Studies have found that supplementation with certain types of probiotics can decrease inflammation and improve skin barrier function through their interaction with gut microbes and immune cells. A healthy intestinal microbiome may help prevent acne formation by improving immunity against harmful organisms and reducing inflammation caused by bacterial overgrowth. This means that taking probiotics could help reduce the severity of acne outbreaks or prevent them altogether by promoting a balanced microbiome that leads to healthier skin.
For example, one study conducted on 20 individuals with acne showed that three months of daily probiotic intake led to significant improvements in skin appearance compared to placebo-controlled participants. Specifically, those who took the probiotic supplement experienced less redness in affected areas and fewer blackheads and cysts than those who received the placebo treatment. These findings suggest that consistent use of probiotics may be an effective way to manage acne.
Studies have shown that certain strains of probiotics can help reduce inflammatory cytokines, improve the immune response, and repair skin barrier function. It is thought that these beneficial effects could translate into reduced acne formation or severity. However, it’s important to note that not all probiotics are created equal, and certain strains may significantly impact acne more than others.
Some experts argue that the research on probiotics and acne is still in its early stages, and more studies would be needed to establish the mechanisms by which these supplements exert their beneficial effects on the skin. Furthermore, some argue that taking probiotics doesn’t necessarily address the root cause of acne formation and should be complemented with a holistic approach to skincare and diet.
Think of probiotics as an army of beneficial bacteria that protect your gut against harmful microorganisms. By supplementing your diet with these beneficial bacteria, you strengthen your internal defenses against potential invaders while also providing building blocks for healthy skin cell production. Just like eating a balanced diet can help prevent disease by giving your body the nutrients it needs to function well, probiotics could also contribute to achieving healthier skin.
Now that we’ve covered the scientific link between probiotics and acne let’s dive deeper into recent research on this relationship.
Research Findings on Probiotics and Acne
There has been growing interest in using probiotics as a supplementary approach to treating various skin conditions in recent years. Several studies have investigated whether consuming adequate amounts of these beneficial bacteria may improve overall gut health, thus reducing multiple skin conditions, including acne.
One study tested the effectiveness of Lactobacillus acidophilus consumption in reducing acne severity over 12 weeks. Results showed that participants who consumed the probiotic supplement experienced a significant reduction in acne outbreak frequency and severity compared to their placebo counterparts. The probiotic supplement also led to a significant decrease in the expression of inflammatory markers in the blood, indicating reduced inflammation.
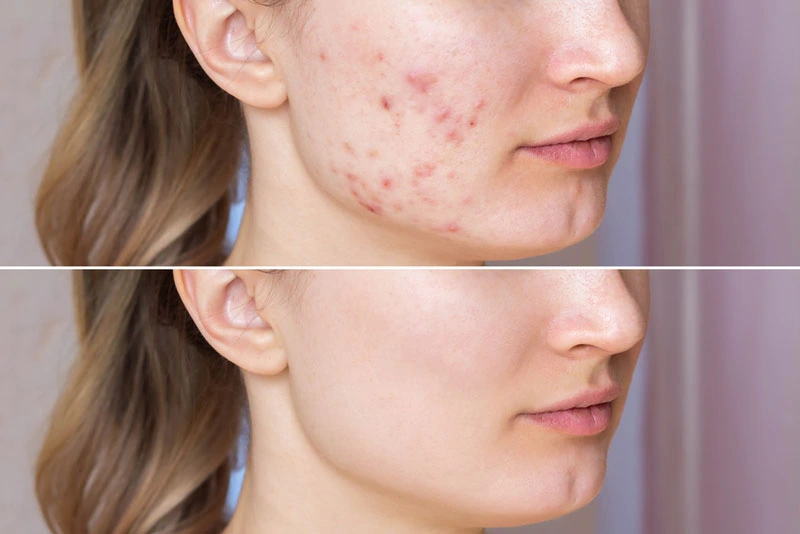
Another study suggested that certain combination probiotics could improve skin hydration and reduce sebum production on the face by inhibiting lipid metabolism enzymes in skin cells. This indicates that probiotics could regulate oil production, repair skin barrier function, and promote overall dermal health.
Additionally, some studies have found that consuming fermented foods containing Lactobacillus acidophilus can significantly reduce inflammatory skin conditions such as psoriasis and eczema. These beneficial bacteria help balance the gut microbiota, decreasing systemic inflammation and improving immune response.
For example, a randomized, double-blind, placebo-controlled study consisting of 56 adults with moderate-to-severe acne vulgaris showed a significant reduction in acne lesions after 12 weeks of probiotic supplementation with the Lactobacillus rhamnosus SP1 strain. Compared to placebo treatment participants, those who took the probiotic supplement exhibited fewer post-inflammatory hyperpigmentation marks and smoother skin texture.
These findings suggest that specific probiotic supplements could improve gut flora health, translating into healthier skin with fewer outbreaks.
However, it is worth mentioning that not all studies have demonstrated favorable results for using probiotics as a complementary approach to treating acne. One study involving 45 patients with moderate-to-severe acne vulgaris failed to show any statistically significant differences between probiotic-treatment or placebos concerning clinical improvement.
Probiotics are like tiny farmers working hard to grow healthy crops inside your body. Like how poor soil quality impacts crop health, a damaged gut microbiome can lead to skin issues such as acne. Using probiotics can be helpful in improving the internal environment of your body by providing what it needs for optimal growth and function.
In the following section, we will explore the role of gut flora in skin health and how using probiotics could have far-reaching benefits beyond just acne management.
The Role of Gut Flora in Skin Health
The gut microbiome is a complex community of microorganisms essential to our health. It consists of trillions of bacteria, fungi, and viruses that reside in the gastrointestinal tract and help break down food, produce vitamins, and regulate the immune system. Moreover, studies suggest that gut health is intimately connected to skin health, and disturbances in gut flora can cause or exacerbate various skin conditions, including acne.
One reason for this link is that the gut and skin share common origins during embryonic development. They are interconnected through a network of nerves, blood vessels, and hormones. Consequently, intestinal imbalances, including the skin, can trigger inflammation throughout the body. For example, when harmful bacteria outnumber beneficial ones in the gut, they can produce toxins called lipopolysaccharides (LPS) that enter the bloodstream and lead to oxidative stress, free radical damage, and inflammation in the skin.
Furthermore, research shows that gut bacteria impact sebum production – the oily substance the sebaceous glands produce that can contribute to acne formation. By interacting with hormones like testosterone and insulin, gut microbes influence the size and activity of these glands. Additionally, certain bacterial strains like Cutibacterium acnes (formerly Propionibacterium acnes) have been linked to acne pathogenesis due to their ability to stimulate an immune response and promote inflammation.
In support of these findings, a small study published in 2019 investigated the effects of probiotics on acne-prone individuals. The researchers found that supplementation with Lactobacillus rhamnosus SP1 reduced inflammatory lesions by 49 percent after 12 weeks compared to placebo.
Another study from 2017 examined the fecal microbiota composition of patients with acne vulgaris compared to healthy controls. The researchers found significant differences in the relative abundance of certain bacterial taxa, including an increase in Staphylococcus and a decrease in Faecalibacterium. Furthermore, they found that the acne patients had higher levels of LPS in their blood, indicating increased intestinal permeability (leaky gut).
However, some experts argue that gut health may contribute to acne, but it is not the sole cause and cannot be treated in isolation. They suggest that other factors like genetics, lifestyle, and skincare habits also play essential roles in acne development and treatment. Moreover, they caution that probiotics may have limited benefits for acne if taken without addressing other aspects of gut health.
To illustrate this point, consider having a leaky faucet in your house. Simply turning off the water flow may temporarily stop the dripping, but it does not fix the underlying issue of a damaged pipe. Similarly, taking probiotics to address gut imbalances may relieve acne symptoms, but it does not address the root causes of the inequality.
Potential Risks of Probiotics
While probiotics are generally safe and well-tolerated by most people, some potential risks are associated with their use. Firstly, since probiotics are live microorganisms, they can interact with medications or other supplements, affecting their efficacy or safety. For example, certain antibiotics can kill beneficial and harmful bacteria, disrupting gut flora’s delicate balance.
In addition to drug interactions, probiotics can cause adverse effects like gas, bloating, diarrhea, or constipation at high doses or when consumed by individuals with compromised immune systems. Furthermore, some probiotics may contain strains that could harm certain populations, like pregnant women or infants.
Moreover, because there is little regulation of the supplement industry concerning the labeling and quality of their products, there may be inconsistencies in the quantity or potency of probiotics listed on the label. Consequently, some people may not respond to a certain probiotic strain due to insufficient dosing or lack of scientific evidence.
However, proponents of probiotics argue that these risks are minimal compared to their potential benefits for gut and skin health. They suggest that people can safely incorporate probiotics into their daily routines by choosing reputable brands and adjusting doses as needed.
To use an analogy, just as we must weigh the risks and benefits of any medication before taking it, we should also consider the potential drawbacks of probiotics before using them. However, if used correctly and responsibly, probiotics can provide many health benefits that outweigh their possible risks.
Complementing Probiotics with Dietary Changes for Acne Management
While probiotics can significantly reduce acne, dietary changes are also crucial for long-term acne management. A healthy diet not only improves your overall health but can also impact the health of your skin. This section will discuss how making small dietary changes and incorporating probiotics into your routine can help manage acne.
Reducing dairy and highly glycemic foods from your diet can benefit acne management. Dairy products like milk contain hormones that cause an increase in sebum production, leading to acne outbreaks. Consuming high-glycemic foods such as white bread and pasta raises insulin levels and can cause inflammation, worsening acne. By limiting these types of foods in your diet, you may see an improvement in your skin complexion.
Additionally, increasing protein intake and consuming more whole foods can positively impact skin health. Protein is essential for collagen production, which helps keep the skin firm and youthful-looking, while whole foods contain vital nutrients essential for healthy skin. Antioxidants in fruits and vegetables protect the skin from damage caused by free radicals, which can decrease inflammation and improve overall skin health.
Some believe that eliminating specific foods like chocolate causes or worsens acne outbreaks. However, research has shown no direct correlation between chocolate consumption and increased acne. That being said, it’s important to note that everyone’s body is different, so it’s essential to pay attention to personal triggers that may lead to breakouts.
Think of taking care of your skin like you would take care of a plant. Just as plants need water and sunlight to grow optimally, our bodies require proper nutrition for healthy skin. Feeding yourself nutrient-rich foods and staying hydrated throughout the day provides your body with the necessary tools to maintain healthy skin.
Lastly, it’s essential to stay hydrated by drinking enough water. When our bodies are dehydrated, less moisture is likely to reach the surface of our skin, leading to dryness and clogged pores which can cause acne. Drinking enough water helps flush out toxins from the body and keeps skin glowing and healthy.
In conclusion, incorporating dietary changes into your acne management strategy can significantly impact your overall complexion when combined with regular probiotic use. While specific foods and triggers vary from person to person, making small dietary changes towards a well-rounded diet that includes whole foods and plenty of hydration can lead to healthy skin and improved overall health.
Answers to Commonly Asked Questions
Is there a difference in effectiveness between oral probiotics and topical probiotic skincare products?
When it comes to treating acne, both oral probiotics and topical probiotic skincare products can be effective. However, their mechanisms of action differ, and therefore they should not be considered interchangeable.
Oral probiotics introduce live bacteria strains into the gut, which can, in turn, modulate the immune system and improve skin health from the inside out. According to a study published in the Journal of the American Academy of Dermatology, oral probiotics significantly reduced the number of inflammatory acne lesions in patients with moderate to severe acne.
On the other hand, topical probiotic skincare products rely on using live bacteria on the skin’s surface to restore balance and promote healthy microbial growth. In a clinical trial reported by Allure, a topical probiotic cream was used and showed a 32% reduction in inflammatory acne after only four weeks of use.
In summary, while oral and topical probiotics have been shown to be effective in treating acne, they operate differently and, therefore, should complement each other rather than replace one another. People with severe acne may benefit more from oral probiotics supplements backed by medical research intervention in addition to maintaining a consistent skincare routine with topical probiotics for optimal results.
Are there any potential side effects or risks associated with using probiotics for acne?
Yes, there are potential side effects and risks associated with using probiotics for acne.
First, it’s essential to note that not all probiotics are created equal. Some strains might cause adverse reactions in some people. According to a study published in the International Journal of Molecular Sciences, Lactobacillus acidophilus, a common probiotic strain found in dairy products, can trigger allergic reactions in some individuals. This could result in skin rashes or hives, exacerbating acne symptoms.
Additionally, probiotic supplements may cause gastrointestinal distress, such as bloating, gas, or constipation. In rare cases, the overgrowth of harmful bacteria can occur, leading to infections, particularly among those with underlying health conditions.
It’s also important to remember that the U.S. Food and Drug Administration (FDA) guidelines do not regulate probiotics. Therefore, the purity and effectiveness of these supplements can vary widely depending on the manufacturer.
In conclusion, while probiotics have shown positive results in treating acne symptoms, it’s crucial to remember that they come with potential risks and side effects. Always consult with your healthcare provider before starting any new supplementation regimen.
How long does it typically take to see results from using probiotics for acne?
If you’re considering using probiotics to treat your acne, one of the inevitable questions is how long it takes to see any noticeable results. Unfortunately, there’s no one-size-fits-all answer to this question, as the time frame to see improvement can vary depending on several factors, such as the severity of acne, the type of bacteria and probiotic strains used, and individual health conditions.
However, research studies suggest that it may take at least 4-12 weeks before any meaningful effects are observed from using probiotics for acne treatment. For instance, a study published in the Journal of Drugs in Dermatology reported that 80% of participants using a topically applied probiotic for 10 weeks saw a reduction in inflammatory acne lesions. Another study carried out by Kim et al. (2019) found that oral intake of Lactobacillus acidophilus for 12 weeks was associated with an overall decrease in inflammatory and non-inflammatory acne.
It’s important to note that maintaining long-term use of probiotics is crucial for continued improvement in skin health based on emerging evidence. A systematic review published in the International Journal of Women’s Dermatology concluded that “a longer duration period (≥8 weeks) of prophylactic use with adequate dosage and quality assurance was more likely to result in a positive clinical outcome.”
In conclusion, while there is evidence supporting the effectiveness of probiotics for treating acne, patience is key to seeing real improvements. It can take up to three months or more before results can be seen, so don’t get discouraged if you don’t experience immediate improvements.
Can adding probiotic foods to your diet also improve acne?
Yes, adding foods rich in probiotics to your diet can improve acne. Research shows that a healthy gut microbiome is crucial for maintaining clear skin, and probiotics can help by balancing the bacteria in your gut. In fact, a 2014 study found that consuming probiotics for just 12 weeks significantly decreased acne severity.
Foods naturally high in probiotics include yogurt, kefir, fermented vegetables (such as sauerkraut and kimchi), and kombucha. Incorporating these foods into your diet can help promote a healthy gut microbiome and may improve acne symptoms.
It’s important to note that while probiotics may benefit some individuals with acne, they are not a cure-all solution. Other factors such as genetics, hormones, and skincare routine also play a role in acne development. As always, it’s best to consult a healthcare professional before making drastic dietary changes or starting a new supplement regimen.
What specific strains of probiotics are effective for treating acne?
When it comes to treating acne with probiotics, certain strains have been found to be more effective than others. Research suggests that Lactobacillus acidophilus, Lactobacillus bifidus, and Bifidobacterium lactis are particularly beneficial for combating skin conditions.
Studies have shown that these strains can reduce inflammation, a key factor in developing acne. They may also help regulate the immune system, reducing the likelihood of a breakout.
One study published in the Journal of Dermatology found that patients who consumed a fermented milk product containing Lactobacillus acidophilus and Bifidobacterium lactis experienced a significant reduction in their acne severity scores compared to those who did not consume the product.
Another study published in the International Journal of Women’s Dermatology found that Lactobacillus fermentum reduced sebum production (excess oil) by 24 percent after four weeks.
Overall, while more research is needed to definitively determine which strains are most effective for treating acne, evidence suggests that these particular strains may hold promise. If you want to incorporate probiotics into your skincare routine, look for products containing these strains or take them as a supplement.




